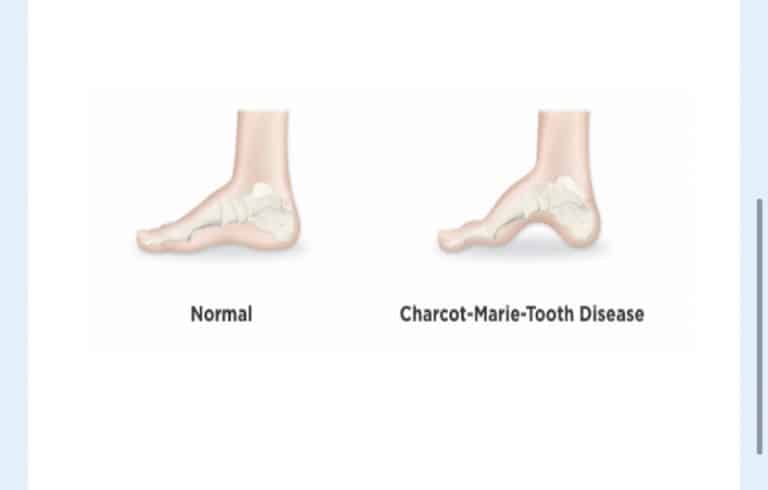
A series of genetic diseases known as Charcot-Marie-Tooth disease (CMT) causes damage to peripheral nerves in the feet. Peroneal muscular atrophy (PMA) and hereditary motor and sensory neuropathy (HMSN) are other names for it. The peripheral nerves are located outside the brain and run down the spinal cord. They relay information from the brain to the rest of the body.
This disease is called “Charcot-Marie-Tooth disease,” which sounds like a dental problem. However, the name comes from the three doctors who first reported the disease in 1886. Charcot-Marie-Tooth disease is one of the most prevalent hereditary nerve illnesses.
Peripheral neuropathy results from nerve injuries to the feet and lower legs. One person in 2500 is afflicted with CMT. Nerve conduction studies can measure the speed and strength of electrical signals passing through the peripheral nerves. Physical and occupational therapy can help but should be started early.
What is Charcot-Marie-Tooth Disease?
Charcot-Marie-Tooth disease is an inherited motor and sensory neuropathy. CMT primarily affects the peripheral nerves in the arms and legs. Charcot-Marie-Tooth will also cause smaller and weaker muscles as the disease progresses.
Due to damaged sensory nerves, problems typically start in the feet and legs and move up to the hands and arms. Genetic counseling can define your level of Charcot-Marie-Tooth disease.
What Causes Charcot-Marie-Tooth Disease?
CMT, also called hereditary motor and sensory neuropathy, is one of the most common inherited neurological conditions. It affects 2.6 million people around the world. In most cases, the disease is a hereditary gene mutation. While Charcot-Marie-Tooth disease can resemble “acquired neuropathy,” nerve damage brought on by diabetes, immunological disorders, inherited nerve diseases, gene defects, or exposure to specific chemicals or substances, a person’s actions do not cause it. It is not a communicable disease.
For a person to move and react quickly and accurately, axons must send messages in a fraction of a second. Motor nerves carry signals long distances, and the peripheral sensory nerves carry sensations to the muscles in the fingers and toes.
The body’s longest nerves are most likely to have axon degeneration, which is why CMT causes motor and sensory problems in the body’s extremities.
What Are the Symptoms of Charcot-Marie-Tooth Disease?
Symptoms of Charcot-Marie-Tooth disease usually start in adolescence or early adulthood, but they can also start in middle age. Charcot-Marie-Tooth disease symptoms can include:
- Weak lower leg muscles, ankles, or feet
- Numbness or a tingling feeling
- Loss of muscle mass in the legs and feet
- High foot arches
- Curled toes (hammertoes)
- Shuffling, or dragging the feet
- Muscle weakness
- Difficulty walking (foot drop)
- Frequent tripping or falling
- Awkward or high steps (gait)
- Decreased sensation or a loss of feeling in the legs and feet
How is Charcot-Marie-Tooth Disease Inherited?
Even when there is no hereditary neuropathy of the disease, the gene mutations of Charcot-Marie-Tooth disease can be passed down from one generation to the next. When a person has mutations in two or more genes, each of which causes a specific form of CMT, and there is a family history, they have an increased chance of developing the illness. The X chromosome is also a factor.
Charcot-Marie-Tooth disease can also damage the protective coating, the myelin sheath, that surrounds the nerves.
Types of Charcot-Marie-Tooth Disease
Different CMT types are labeled by how severe they are, how affected the peripheral nerve cells are, any damage to the myelin sheath, and how they are related to axonal or myelinated abnormalities. The X-linked category and types 1 through 7 of CMT are the main subcategories. Also, the level of the gene mutation from one or both parents can determine which type of CMT you have.
CMT1
CMT1 causes muscle atrophy and can lead to recurrent ankle sprains and sensory abnormalities (paresthesia), which make people clumsy, slow, or cause them to fall. This type of CMT usually starts in childhood and affects nerves in the extremities of the body, like the feet, lower legs, hands, and forearms. People who have severe symptoms of CMT1 may also have sleep apnea or other breathing difficulties.
CMTX
Many of the symptoms of CMTX share those of CMT1 and CMT2, such as muscular atrophy and weakening as well as alterations in sensation, mainly in the hands, forearms, feet, and lower parts of the legs. Because CMTX is linked to the X chromosome, this gene mutation affects men more often than women.
CMT4
Symptoms of CMT4 are worse than those of CMT1 or CMT2, and they usually affect the muscles near the center of the body. Some people may also lose their sense of touch or their ability to notice temperature changes, while others may get cataracts or lose their hearing.
CMT2
CMT2 can cause weakness, atrophy, decreased deep tendon reflexes, loss of sensation, and different foot deformities. Usually, symptoms manifest between the ages of 5 and 25, which is later than in CMT1.
Severe, early-onset CMT
Starting in infancy, slow or no reflexes, weakness, low muscle tone, sensory loss, delayed motor development, and profoundly slowed nerve conduction are all symptoms of severe, early-onset CMT.
CMT 5, 6, and 7
Due to its genetic cause, CMT5 symptoms are sensory neuropathy or a partial loss of mobility in the lower limbs. People with dominant or recessive optic atrophy and motor-sensory neuropathy are diagnosed with CMT6. And people with both motor-sensory neuropathy and retinitis pigmentosa, an eye disease that affects the retina, have CMT7.
Intermediate CMT
The least common CMT type is known as intermediate CMT. Doctors use this name when the symptoms are not clearly defined.
How Does Charcot-Marie-Tooth Disease Affect Your Brain and Spinal Cord?
CMT does not directly affect the brain or spinal cord. Because it damages the nerves located outside of the brain and spinal cord, it is called “peripheral neuropathy.” However, some patients have reported minor memory loss.
What is the Treatment for Charcot-Marie-Tooth Disease?
While there is currently no cure for CMT, doctors can control the symptoms to a certain extent.
Physical Therapy
In physical therapy, patients perform low-impact exercises with the help of a therapist, like swimming, biking, and aerobics, to stretch and strengthen muscles and help revive nerve signals. Doctors advise patients to remain active to slow muscle weakness.
Occupational Therapy
Patients with Charcot-Marie-Tooth disease may find it challenging to carry out daily duties if the disease has spread to the arms and hands. Seek training from a specialist to increase flexibility, strength, and grip to maintain your lifestyle.
Orthopedic Devices
Orthotics, such as leg braces, ankle braces, and other devices, can help with movement and support.
Pain Medicines
Talk to your doctor about medications that can make muscle spasms or nerve damage less painful.
How Can Cutting Edge Clinic Help?
Cutting Edge Foot and Ankle Clinic is a specialty clinic that treats all kinds of foot and ankle problems. If you think you are experiencing any CMT symptoms, call us right away. We are a great place for you to get help so you can get back to your normal activities.
What Services Does Cutting Edge Foot and Ankle Clinic Provide?
Besides treating CMT, we also offer these services:
• Skin Conditions
• Foot Deformities
• Heel Pain
• Plantar Warts
• Achilles Tendinitis
• Flatfoot Issues
• Bunions
• Morton’s Neuroma
• Diabetic Foot Care
How Do I Take Care of Myself?
While most neurological disorders cannot be cured, doctors can effectively manage its symptoms with specialized treatments and counseling. Even with a family history of CMT, many people can lead active, useful lives with treatment and medication.
1. See your provider as recommended
The first course of treatment for CMT entails collaboration with a physical or occupational therapist to control muscle weakness and decreased sensitivity.
2. Follow your treatment plan.
Follow your doctor’s recommendations about diet, exercise, and medications. Remain active to avoid progressive muscle weakness.
3. Avoid drugs or neurotoxicity
Do not take any medications or other drugs without your doctor’s knowledge. Your doctor can give you a list of drugs that may worsen your condition.